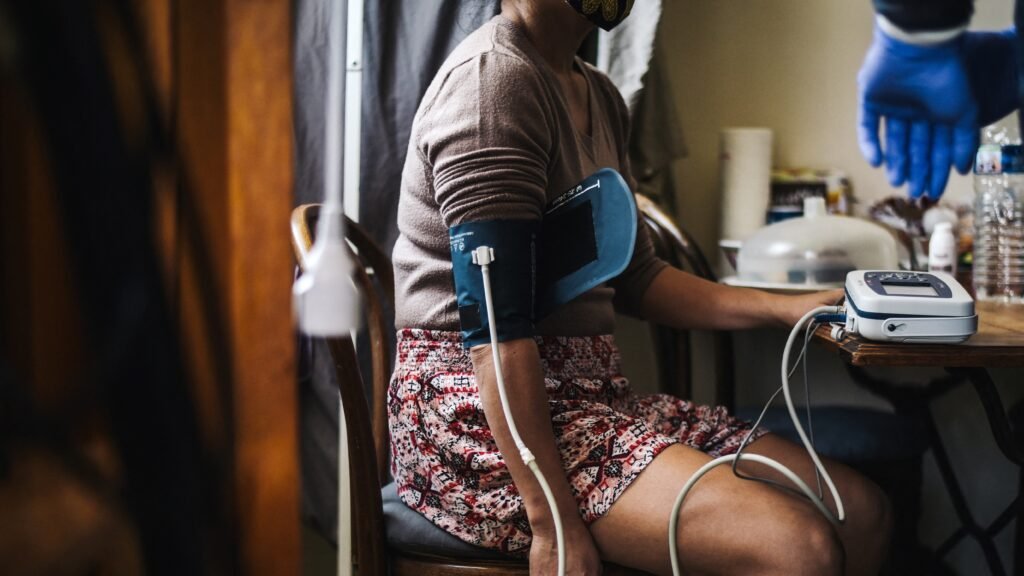
It’s the leading risk factor for the leading cause of death in the United States and around the world: high blood pressure, the prime mover in heart attacks and strokes.
High blood pressure is treatable, but despite having access to effective and affordable medications, more than half of Americans still have uncontrolled hypertension, with rates going up in sync with adverse social determinants of health.
A new study tested what else might work beyond well-established drug regimens for patients of low income with high blood pressure. The strategy: A team-based, protocol-driven approach that included home monitoring and feedback, medication adjustment, and health coaching from primary care providers, nurses, and community health workers.
The results: significantly lower blood pressure readings compared to patients randomly assigned to “enhanced” usual care at 36 federally qualified health centers in Louisiana and Mississippi. (Enhanced care meant physicians were educated about clinical guidelines for hypertension.) The study followed patients for 18 months, overlapping the emergence of Covid-19 and its disruptions to health care.
Dan Jones, a cardiologist who led the team developing the American Heart Association’s latest blood pressure guidelines, called the study “really, really important” and a big win for exploring ways to improve blood pressure control.
“It takes team-based care and applies it in probably one of the most difficult clinical settings that you can find in the United States: federally qualified community health centers in two of the poorest states in the nation,” he told STAT. Past president of the American Heart Association and dean emeritus of the University of Mississippi School of Medicine, Jones was not involved in the new research. “They didn’t plan on the pandemic, but there it came. And so they had really difficult circumstances to try to prove the point — and they proved the point.”
For decades, keeping the top blood pressure number under 140 mm Hg was the goal, but more recent research from the Systolic Blood Pressure Intervention Trial, or SPRINT, showed that a lower target — under 120 mm Hg — greatly reduced heart attacks, heart failure, and strokes as well as deaths from all causes.
The study, published Wednesday in the New England Journal of Medicine, is the first randomized controlled trial to test and implement the multifaceted, intensive strategy to improve hypertension control in low-income patients, co-author Jiang He, chair of epidemiology and professor of internal medicine and neurology at UT Southwestern, told STAT in an interview. That intensive treatment protocol relied on principles from the SPRINT trial.
Teams monitored and adjusted care (including medications), patients checked their blood pressure at home and shared readings with the team at least three times a week for feedback, and community health workers coached patients on how to stay on their medications and make lifestyle changes.
More than 1,200 patients with uncontrolled hypertension were randomly split into two groups. Half received usual care, visiting a doctor trained on new hypertension guidelines every four to six months. The other half got the SPRINT team approach, which started with monthly visits to make medicine adjustments. Most participants were already taking blood pressure medications. Their average age was 59, a little more than half were women, and nearly two-thirds were African American. Three-quarters were unemployed and about the same proportion had a family income of less than $25,000 per year.
It was challenging to bring patients back for their routine clinic visits, co-author He said, and it wasn’t easy for patients to buy and stay on their medications.
“Many patients have to choose between buying food and purchasing medications, given their limited resources,” he said.
That’s where health coaches, including nurses or medical assistants, came in, helping patients apply for medication assistance programs that allowed them to afford and stay on their medications.
Over 18 months, patients in team-supported care reduced their top blood pressure number by an average of 16 mm Hg, while the control group had a 9 mm Hg reduction. The team group also scored higher on adhering to their blood pressure management plan. The two groups reported similar levels of serious side effects. The average implementation cost for the team group was $762 per patient.
Co-author Marie Krousel-Wood, associate provost for the health sciences at Tulane University, said the results were similar to those from other studies done at Kaiser Permanente and Veterans Affairs using multicomponent system-level interventions, including protocol-based treatment, to improve hypertension control. “It is good news that this team-based, multifaceted approach in this unique setting that included rural and urban clinics in federally qualified health centers in low-resourced and underserved populations did translate into lower blood pressure compared to the control group, even in patients already taking medications, but still had uncontrolled blood pressure in real world clinical settings,” she said in an interview.
Tom Frieden, president and CEO of the global nonprofit Resolve to Save Lives and former director of the Centers for Disease Control and Prevention, praised the trial for translating the SPRINT findings to the groups that could benefit most. And he pointed out that people in the control group also improved, showing that even modest investments in enhanced routine care can pay off.
“The real question is why the U.S. health care system does so poorly at blood pressure control, which can prevent more deaths than any other clinical intervention,” he said via an email to STAT about prevention versus treatment. “Most of American health care operates on the opposite incentive: A heart attack is a revenue event. Until we fix that, trials like this will remain islands of progress in a sea of inaction.”
An editorial published along with the NEJM study said the findings offer “much-needed evidence for systems-based strategies” that can be successful in community health centers. It also called the difference in blood pressure between the intervention and control groups “modest” and the effort to get there costly.
“We can and must do better for our patients and communities as we continue to bridge the gap between evidence-based therapies and routine clinical practice to improve blood-pressure control and improve cardiovascular, kidney, and brain health for all,” Sadiya Khan of the Northwestern University Feinberg School of Medicine and Mark Huffman of the Washington University School of Medicine wrote.
In response, study co-author He said, “In this low-income population, we achieved blood pressure control with a systolic level below 130 mm Hg in 47.7% of patients. In contrast, only 22% of patients in the U.S. general population reach this target. … This means blood pressure reduction has important public health implications.”
The researchers hope to scale up the study beyond Louisiana and Mississippi and conduct an economic analysis, He said. Jones would like to see the work encourage change at the health system level.
“This is not something that an individual physician or clinician can make a decision to do,” he said.
STAT’s coverage of chronic health issues is supported by a grant from Bloomberg Philanthropies. Our financial supporters are not involved in any decisions about our journalism.