The reports emerging this week of a major Ebola outbreak in the Democratic Republic of Congo, coming alongside a growing hantavirus outbreak linked to a cruise ship in South America, should serve as another warning that the era of emerging infectious diseases is not ahead of us. We are already living in it.
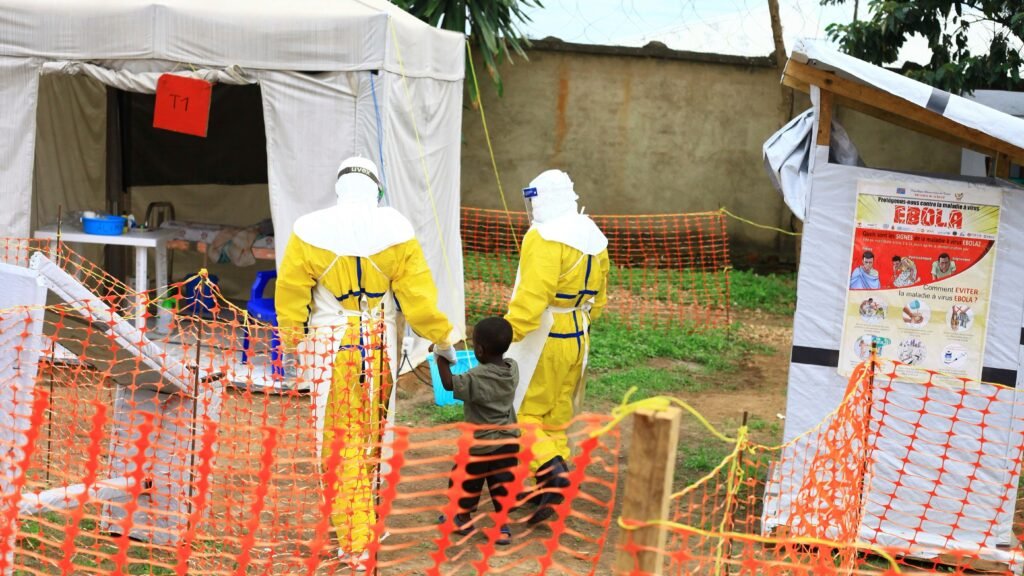
According to Africa CDC, the Ebola outbreak in Ituri province has already resulted in 246 suspected cases and 65 deaths, with preliminary testing suggesting a non-Zaire ebolavirus strain. The agency has raised concerns about spread driven by population movement, political and health insecurity in affected areas due to violence, gaps in contact tracing, health care-associated transmission, and limited infection prevention and control capacity.
At the same time, public health authorities in Argentina are investigating the well-publicized hantavirus outbreak associated with a cruise ship, raising difficult questions about international travel, delayed recognition of unusual illnesses, and cross-border coordination.
These outbreaks are biologically different, geographically distant, and epidemiologically unrelated. But together they reveal something deeply important about the current state of global health: Outbreaks are becoming more frequent, more complex, and increasingly difficult to contain in a world that is less prepared than it should be.
For years, experts warned that Covid-19 would not be the last major infectious disease crisis of our lifetimes. Yet only a few years later, the world appears to be moving in the opposite direction of preparedness. Public health funding is under strain. Trust in health institutions has eroded. Global coordination mechanisms are increasingly challenged by geopolitical tensions. In some countries, scientific expertise itself has become politicized.
At the same time, the conditions that drive infectious disease emergence continue to intensify. Climate change is altering vector ecology and animal migration patterns. Conflict and displacement are disrupting health care systems and vaccination programs. Urbanization and global travel allow pathogens to move faster than ever before. Human encroachment into wildlife habitats continues to increase opportunities for spillover events.
And perhaps most concerning, many outbreaks are now unfolding in environments already weakened by overlapping crises and political and health insecurity leading to fragile health infrastructure, workforce shortages, misinformation, and limited laboratory capacity.
The new Ebola outbreak in eastern DRC illustrates this clearly. Outbreak response in the region has long been complicated by armed conflict, distrust, and logistical barriers. Health care workers and laboratory personnel are themselves among the casualties. These are not simply biomedical events; they are humanitarian and systems-level crises.
The hantavirus outbreak highlights another challenge: Even pathogens that are relatively rare can quickly generate international concern when they intersect with travel, tourism, and interconnected health systems. In a globally connected world, outbreaks that begin in remote settings rarely stay isolated for long.
These events also underscore the critical importance of international organizations such as the World Health Organization and regional bodies like Africa CDC. Rapid information sharing, coordinated technical guidance, laboratory support, deployment of experts, and cross-border collaboration are essential during outbreaks. Global health emergencies cannot be managed by countries acting alone. Weakening international public health institutions at a time of increasing infectious disease threats risks leaving the world more fragmented, slower to respond, and ultimately less safe.
The lesson is not that panic is warranted. It is that preparedness cannot be reactive.
Preparedness is not built during a crisis press conference or after a pathogen has already crossed borders. It requires sustained investment in surveillance systems, laboratory networks, infection prevention and control, health care workforce training, risk communication, and international coordination long before emergencies occur. It requires strengthening institutions even when outbreaks are no longer dominating headlines.
Importantly, preparedness also means recognizing that global health security is collective. An outbreak anywhere can become a threat everywhere if detection, reporting, and response systems are weak. Supporting countries facing outbreaks is not charity; it is a core component of international stability and security.
As mass gatherings such as the FIFA World Cup approach, these conversations become even more relevant. Large-scale international events do not create infectious disease threats, but they can expose vulnerabilities in surveillance, coordination, and health care readiness. The question is not whether another outbreak will occur. It is whether the world has learned enough from recent years to respond more effectively when it does.
Right now, the answer remains uncertain.
Krutika Kuppalli is an infectious diseases physician in Dallas. Her work focuses on emerging infectious diseases, outbreak response, vaccine policy, and clinical care of complex infections. She has extensive experience with Covid-19, mpox, and Ebola, including working for the World Health Organization.